High-Functioning ADHD: Why the Term Is Misleading, What DSM Presentations Actually Mean, and What to Do If Your ADHD Is "Hidden"
- Kiesa Kelly

- 7 days ago
- 10 min read
Last reviewed: 4/19/2026
Reviewed by: Dr. Kiesa Kelly

"High-functioning ADHD" is one of those phrases that became popular because people needed language for a real experience — holding down a demanding job, keeping up with life on the outside, while quietly burning through every reserve you have just to maintain it. The phrase describes something real. It is also not a clinical term, and using it as if it were can lead to some of the worst missed diagnoses in adult mental health: people who clearly meet criteria but decide they cannot possibly have ADHD because they have "done too well" in school or at work.
This guide explains what "high-functioning ADHD" usually means in practice, what the DSM actually says about ADHD presentations and severity, how hidden ADHD shows up, when it starts to fall apart, and what a reasonable next step looks like.
In this article, you'll learn:
Why "high-functioning ADHD" is not a formal diagnosis — and what the DSM describes instead
What the term usually means in lived experience
How ADHD hides, especially in women and AFAB adults
The life events that unmask hidden ADHD
When a screener is enough, and when to consider a full assessment
Is "high-functioning ADHD" a real diagnosis?
Short answer: no. "High-functioning ADHD" is not a recognized term in the DSM-5-TR, the ICD-11, or any current clinical practice guideline. It is a popular description, not a diagnostic category [1]. Clinicians may use it conversationally, but a formal assessment report will not list "high-functioning ADHD" as a diagnosis.
If you are weighing whether to pursue assessment, our overview of psychological assessments explains how diagnostic evaluation actually works.
What the DSM actually describes — presentations, not severity levels
The DSM-5-TR defines ADHD as a neurodevelopmental disorder with three presentations:
Predominantly inattentive presentation — the person meets enough inattention criteria but not enough hyperactive-impulsive criteria
Predominantly hyperactive-impulsive presentation — the reverse
Combined presentation — enough criteria are met on both sides

ADHD also has severity specifiers — mild, moderate, or severe — that describe the intensity of symptoms and functional impairment [1]. None of these specifiers is "high-functioning." In clinical language, someone who meets criteria but whose impairment is subtle is more accurately described as having mild-severity ADHD, predominantly inattentive presentation — or combined presentation with strong compensatory strategies.
This distinction matters because "high-functioning" as a casual phrase often collapses two very different things: external performance and internal cost. The DSM description keeps them separate.
Why the label became popular and where it falls short
The label became popular because ADHD stereotypes — the restless, visibly distracted schoolchild — never matched the experience of many adults, especially women and AFAB adults, whose presentations tend to be inattentive, internalized, and carefully masked [2]. "High-functioning ADHD" was a way to say: "I'm not that stereotype, but something is still going on."
Where the label falls short: it can create a self-image that blocks help. If you think you need to be visibly failing to have ADHD, you will likely wait years past the point where treatment would have helped.
Key takeaway: 🏷️ "High-functioning" describes what others see from the outside. DSM criteria describe what is happening internally. A careful adult ADHD evaluation looks at both — because both matter, and the discrepancy between them is often the clearest sign.
What "high-functioning" usually means in practice
High external performance, high internal cost
For most adults who identify with the term, "high-functioning ADHD" describes a specific pattern: you have looked capable to colleagues and family for years — deadlines met, promotions earned, kids cared for — and you also know, privately, what that has cost. You have traded sleep, weekends, relationships, hobbies, health. You have lived in a near-constant state of low-grade overwhelm, and the gap between "how I appear" and "how I actually am" has become its own exhausting performance.
Key takeaway: 💼 The phrase "functioning well" usually means "succeeding at visible outputs." Someone with hidden ADHD can be functioning on every external metric while their internal experience — exhaustion, self-criticism, constant compensation — would warrant treatment on its own.
The compensation strategies that eventually break down
The specific strategies are recognizable once they are named. You may:
Rely on deadline pressure and adrenaline to force yourself into tasks you would otherwise not start
Over-commit in the morning when energy feels high, then burn out by afternoon
Use public commitment ("I'll have it for you tomorrow") as an external pressure system
Keep elaborate external calendars, lists, and reminders that absorb most of your cognitive bandwidth
Overfunction in bursts to compensate for long stretches of inertia
These strategies work — for a while, at a cost. The cost tends to be invisible until a life event raises the overall load enough that the strategies can no longer absorb the difference.
How hidden ADHD shows up
Inattentive presentation — the pattern most often missed
The inattentive presentation is the one most often overlooked in adults. It looks like:
Starting tasks is nearly impossible until consequences feel urgent
Sustaining attention on boring-but-important work is costly in a way that does not fade with experience
You lose track of conversations, meetings, and what you were doing five minutes ago
Forms, follow-up emails, scheduling, errands — the administrative layer of life — gets put off until small problems become crises
Your working memory may look fine when tested in a quiet room but quietly breaks down in daily life
A worked example: You are widely considered dependable at work. You are also the person who misses small internal deadlines, forgets to register for the conference you wanted to attend, and reliably pays a late fee on the same bill three times a year. Your desk has three half-finished projects, and you know exactly what each one needs — you just cannot make yourself sit down and do it. You have organized your life to put external pressure on everything important, and that system is the reason you function at all.
Or: You are the partner in your household who carries the mental load for logistics, and also the partner who forgets the pediatrician appointment every time. You feel the friction of that contradiction every day. You are not unreliable. You are running a brain that is very good at problem-solving and very bad at task maintenance.
Working memory and executive-function strain
ADHD is fundamentally a disorder of executive function, not attention alone [3]. The executive-function costs often show up as:
Difficulty holding multi-step instructions in mind while executing them
Losing track of what you were doing when you opened a new tab
Difficulty prioritizing when everything feels equally urgent
Mental fatigue after work tasks that do not feel proportionate to the tasks themselves
Our ESQ-R executive function screener is a validated self-report instrument designed specifically to measure everyday executive function — the stuff that is often missed by formal cognitive testing in a quiet room.
Emotional regulation and rejection sensitivity
ADHD is also a regulation disorder. Emotional intensity, difficulty shifting out of an emotion once it arrives, and heightened sensitivity to perceived rejection are commonly reported by adults with ADHD, though "rejection-sensitive dysphoria" is a descriptive term rather than a formal diagnostic criterion [4]. These features often sit at the heart of what "high-functioning ADHD" actually feels like from the inside.
Late-diagnosed ADHD in women and AFAB adults
Women and AFAB adults are disproportionately diagnosed late — often after a child's diagnosis makes their own pattern obvious, or after a life transition unmasks it [5]. Research into sex and gender differences in ADHD presentation and diagnosis is an active and still-developing area [5][6]. Common late-diagnosis paths include a perimenopausal symptom increase, a job change that removes the structure that was holding things together, or the birth of a child whose needs exceed the parent's compensatory bandwidth.
Misconception: I got good grades and went to a good school, so I can't have ADHD. In reality, intellectual ability and ADHD are independent. High cognitive ability often lets someone compensate for ADHD for years — through intense cramming, deadline adrenaline, or interest-driven bursts of focus — without removing the underlying impairment.
Misconception: If I can hyperfocus, it can't be ADHD. Hyperfocus is common in ADHD. ADHD is about difficulty regulating attention — including the capacity to shift out of an intense focus — not a simple deficit of it.
Misconception: ADHD is overdiagnosed right now, so probably I don't really have it. The current research evidence does not support a broad overdiagnosis narrative in adults; rather, the field is catching up on decades of underdiagnosis in adults, especially women and AFAB adults [5]. Evaluating yourself based on media framing is not how this question is meaningfully answered — evaluating yourself based on lived symptoms and functional impact is.
When high-functioning ADHD starts to fall apart
Life transitions that unmask it
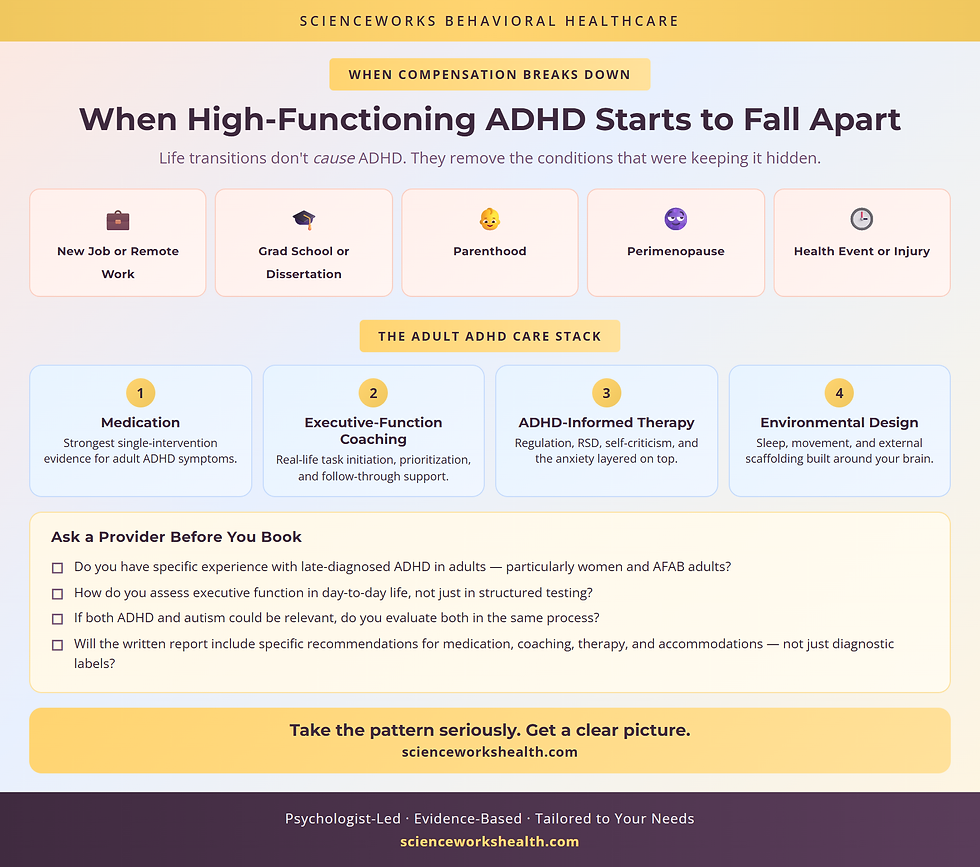
Hidden ADHD often becomes visible at moments when the overall demand load increases faster than compensatory strategies can scale. The most common:
A new job with less structure or higher independent initiation (remote work frequently unmasks ADHD)
Graduate school, especially dissertation-stage work where the deadline structure thins
Parenthood — especially with a young child whose needs cannot be deferred
Perimenopause — hormonal shifts affecting attention and executive function
A health event or injury that removes the compensatory energy reserves you were running on
None of these causes ADHD. They remove the conditions that were keeping it hidden.
Burnout, anxiety, and misattributed "just stressed" framing
When the compensation fails, the first wave of symptoms often looks like anxiety, depression, or burnout. Many adults spend years being treated for those before anyone asks the ADHD question. Treatment for anxiety or depression may help some of the secondary symptoms without addressing the underlying executive-function and regulation differences, which tends to produce partial improvement that stalls.
Key takeaway: 🌡️ Treatment-resistant anxiety or depression in a high-achieving adult is worth a second look for ADHD. It is one of the most common paths to an adult diagnosis.
What to do if you suspect hidden ADHD
Start with a screener
The ASRS is a well-validated ADHD screener for adults, developed with the World Health Organization [7]. The ESQ-R complements it by measuring everyday executive function. Together they give you a clearer picture than either one alone.
A screener cannot diagnose ADHD, but a clearly elevated ASRS — especially paired with a full picture of functional impact — is a strong signal to consider a formal evaluation.
When to pursue a full psychological assessment
Consider a full evaluation when: screeners are elevated, the pattern has been present for years, it is affecting work or relationships, prior treatment for anxiety/depression has only partially helped, or you need documentation for medication, workplace accommodations, or graduate school.
A full evaluation looks at the full clinical picture — ADHD alongside autism, anxiety, depression, and trauma when relevant — and produces a written report with specific recommendations. When combined autism and ADHD is plausible, a combined AuDHD-capable evaluation is often the most useful single assessment.
How coaching and therapy work alongside (or in place of) medication
Medication is the most consistent intervention for ADHD symptoms in adults, with strong evidence across decades of research [8]. But medication is not the only tool. Many adults benefit from executive-function coaching, ADHD-informed therapy, and lifestyle structures (sleep, movement, external scaffolding) alongside — or in some cases instead of — medication. The right combination depends on symptom profile, life situation, and preferences.
Key takeaway: 🧰 Effective adult ADHD care is usually a stack — medication, coaching, therapy, and environmental design working together. A good evaluation should point to specific tools, not just confirm a label.
Questions to ask a provider before booking
Do you have specific experience with late-diagnosed ADHD in adults, particularly in women and AFAB adults?
How do you assess executive function in day-to-day life, not just in structured testing?
If my picture suggests both ADHD and autism could be relevant, do you evaluate both in the same process?
What will the written report include — specific recommendations for medication, coaching, therapy, and accommodations, or only diagnostic labels?
Frequently asked questions about high-functioning ADHD
Is "high-functioning ADHD" listed in the DSM?
No. ADHD in the DSM-5-TR is described by presentation (inattentive, hyperactive-impulsive, combined) and severity (mild, moderate, severe) — not by "high-functioning" as a modifier.
Can I have ADHD if I graduated from a demanding program?
Yes. Intellectual ability and ADHD are independent. High ability often delays diagnosis by letting the person compensate for years before the strategies break down.
Is adult ADHD real, or just a trend?
Adult ADHD is well-established in the research literature and recognized by every major diagnostic system [1][8]. Adult diagnosis rates have risen in recent years largely because the field is catching up on historical underdiagnosis in adults, especially women.
Do I need medication to treat adult ADHD?
Medication has strong evidence, but it is not the only option. Many adults use a combination of medication, therapy, executive-function coaching, and environmental design. The right mix is individualized.
Next step: explore ADHD assessment and executive-function coaching
If "high-functioning ADHD" describes your lived experience, the most useful next step is to take the pattern seriously and get a clear picture. Start with the ASRS and ESQ-R, and if they are elevated, contact us to talk about assessment. If a full evaluation is not the right fit yet, executive-function coaching can often start producing traction while you decide.
About the Author
Dr. Kiesa Kelly is a licensed clinical psychologist and the founder of ScienceWorks Behavioral Healthcare. Her clinical training took place at the University of Chicago, Vanderbilt University, and the University of Wisconsin, with more than twenty years of experience in psychological assessment and evidence-based treatment for adults and adolescents. She has particular expertise in late-identified ADHD, autism, and combined AuDHD profiles, especially in women and AFAB adults whose presentations were missed in earlier life.
Dr. Kelly's approach emphasizes that "high-functioning" is usually a description of cost tolerance, not symptom severity — and that a thorough assessment produces recommendations that make everyday life actually easier, not just a label that explains why it has been hard.
References
1. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th Edition, Text Revision (DSM-5-TR). 2022. https://www.psychiatry.org/psychiatrists/practice/dsm
2. Quinn PO, Madhoo M. A review of attention-deficit/hyperactivity disorder in women and girls: uncovering this hidden diagnosis. Primary Care Companion for CNS Disorders. 2014;16(3):PCC.13r01596. https://doi.org/10.4088/PCC.13r01596
3. Barkley RA. Executive Functions: What They Are, How They Work, and Why They Evolved. Guilford Press; 2012. https://www.guilford.com/books/Executive-Functions/Russell-Barkley/9781462505357
4. Beheshti A, Chavanon ML, Christiansen H. Emotion dysregulation in adults with attention deficit hyperactivity disorder: a meta-analysis. BMC Psychiatry. 2020;20(1):120. https://doi.org/10.1186/s12888-020-2442-7
5. Attoe DE, Climie EA. Miss. Diagnosis: a systematic review of ADHD in adult women. Journal of Attention Disorders. 2023;27(7):645-657. https://doi.org/10.1177/10870547231161533
6. Young S, Adamo N, Ásgeirsdóttir BB, et al. Females with ADHD: an expert consensus statement. BMC Psychiatry. 2020;20(1):404. https://doi.org/10.1186/s12888-020-02707-9
7. Kessler RC, Adler L, Ames M, et al. The World Health Organization Adult ADHD Self-Report Scale (ASRS): a short screening scale for use in the general population. Psychological Medicine. 2005;35(2):245-256. https://doi.org/10.1017/S0033291704002892
8. National Institute for Health and Care Excellence. Attention deficit hyperactivity disorder: diagnosis and management (NG87). 2019. https://www.nice.org.uk/guidance/ng87
9. Faraone SV, Banaschewski T, Coghill D, et al. The World Federation of ADHD International Consensus Statement. Neuroscience and Biobehavioral Reviews. 2021;128:789-818. https://doi.org/10.1016/j.neubiorev.2021.01.022
10. Asherson P, Buitelaar J, Faraone SV, Rohde LA. Adult attention-deficit hyperactivity disorder: key conceptual issues. The Lancet Psychiatry. 2016;3(6):568-578. https://doi.org/10.1016/S2215-0366(16)30032-3
Disclaimer
This article is for informational and educational purposes only and is not a substitute for medical advice, diagnosis, or treatment from a licensed clinician. Reading this article does not create a clinical relationship with ScienceWorks Behavioral Healthcare. If you are in crisis or need immediate support, contact the 988 Suicide and Crisis Lifeline or your local emergency services.



